Introduction: Avoiding postoperative cerebrospinal fluid (CSF) leaks remains a paramount objective of endonasal tumor surgery. The authors previously published their graded repair technique for skull base closure after endonasal surgery in both the microscopic (Esposito 2007) and endoscopic (Conger, Zhao 2018) settings. As this technique has evolved in the endoscopic era, the authors have gained appreciation of the need for precision placement of nasal/sphenoid packing to minimize the risk of repair construct migration and repair failure. Herein, the authors present a direct visualization technique for placement of temporary nasal packs (Merocel, Medtronic ENT) as a soft buttress to augment closure and prevent cerebrospinal fluid (CSF) leaks in endoscopic endonasal tumor removal.
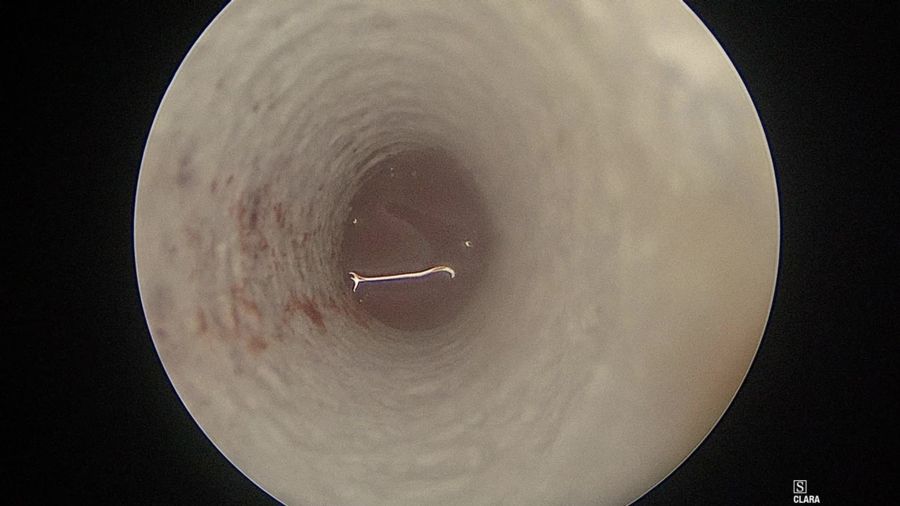
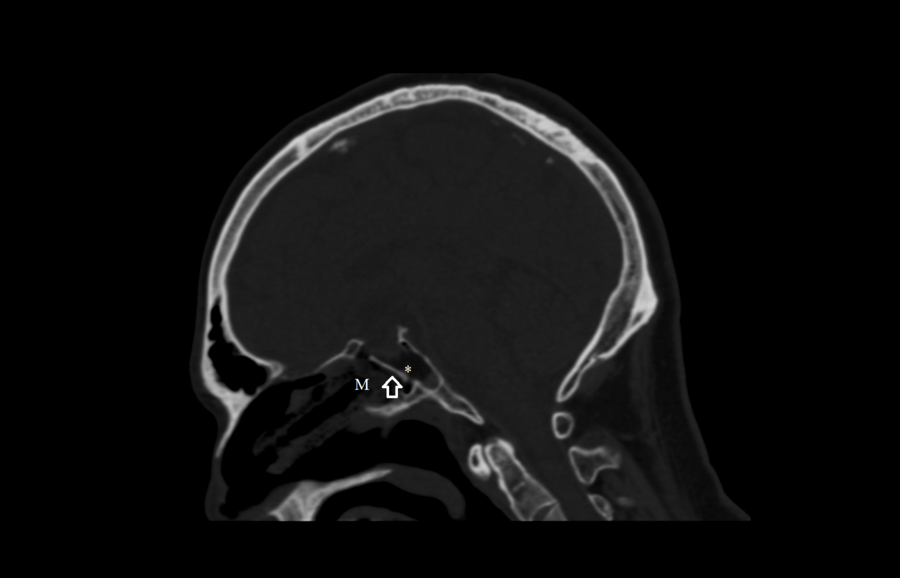
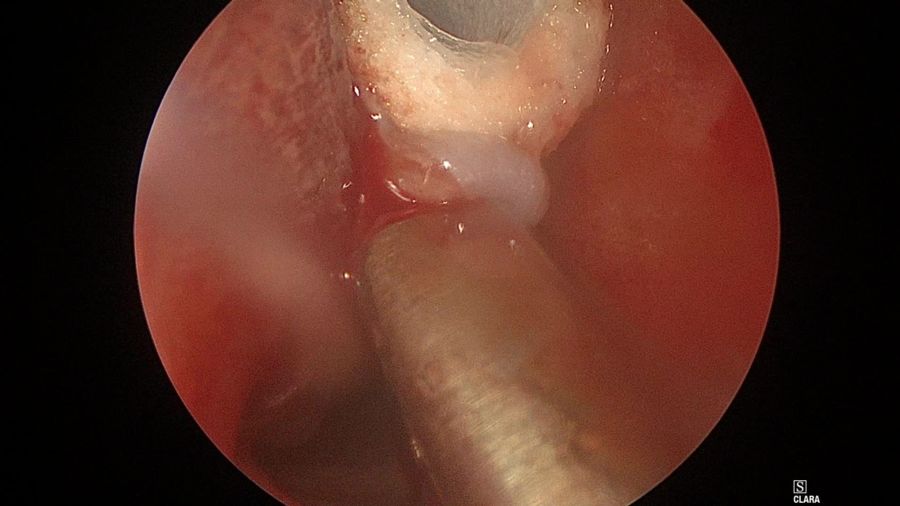
Methods: After tumor removal and skull base closure, if a rigid buttress cannot be effectively wedged into a sellar defect, and in all cases of use of a pedicled nasoseptal or middle turbinate flap, one or two Merocel packs are placed up to the skull base reconstruction within the sphenoid sinus under direct visualization. The Merocel is placed over the endoscope shaft, and the endoscope and Merocel are then inserted together through the nostril (Fig 1). Under direct visualization, the Merocel is then slid off the endoscope up to the reconstruction within the sphenoid sinus, typically up to the face of the sella. The endoscope is then withdrawn, while the distal end of the Merocel is gently wedged against the reconstruction (Fig 2). Placing the Merocels more superiorly in the nasal cavity allows airflow and nasal breathing. A post-operative CT scan is obtained within 1-2 hours of surgery to assess the reconstruction (Fig 3). The packs are removed in the clinic 5 or 6 days post-surgery.
Results: This technique was used in 127 of 551 operations (23%) including in 6 (2%), 16 (16%),31 (32%), and 74 (89%) of Grade 0, 1, 2, and 3 leaks, respectively. The most common pathologies in which this technique was used were pituitary macroadenoma, meningioma and craniopharyngioma. Lumbar drains were not used intraoperatively. Repair failures occurred in 4 of 127 (3.2%) operations using the Merocel technique versus 5 of 424 (1.2%) without Merocel. The four Merocel technique failures occurred in one grade 2 and three grade 3 leaks. In the entire series of 551 operations, the aggregate repair failure rate for all grade 2 and 3 leaks (n=181) was 3.9%. Repair failure rates for all Grade 2 and 3 leaks with and without Merocel were 4/101 (4%) and 3/73 (4%) respectively. Most patients reported the ability to breathe through their noses while still in the hospital.
Conclusions: In this series, direct placement of a soft temporary Merocel sinonasal buttress appears to be an effective adjunct to prevent graft migration, particularly for higher grade leaks. Instead of blindly placing a temporary buttress, this simple technique helps ensure stability of the skull base reconstruction, and augments the standard layered closure, reducing the risk of CSF leak while still maintaining a patent airway for most patients in the acute post-operative period.